If it’s not clear to your doctor—or you—whether you should take a statin to lower your blood cholesterol, finding out your coronary artery calcium score, or CAC, may help close the uncertainty gap. It’s done with a quick CT scan.
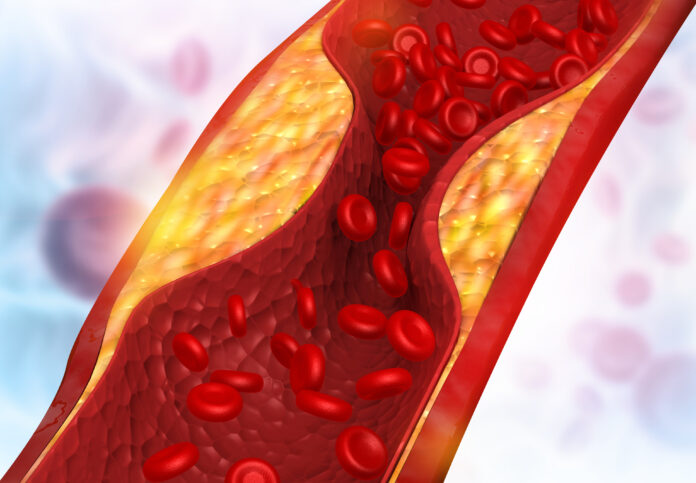
Your cholesterol level tells you how much cholesterol is circulating in your blood. But it doesn’t tell how much cholesterol-laden plaque has actually developed in the walls of your blood vessels, which is what increases the risk of a life-threatening cardiovascular event. A CAC scan provides a much more direct measure of the degree of any plaque accumulation.
The test is not recommended for everybody. Often, the risk for heart disease is high enough that it’s clear a statin should be prescribed to lower blood cholesterol. Or it’s low enough that it’s clear a statin is not needed. But for people 40 through 75 who are determined to be at intermediate risk of heart disease based on their score on the Heart Risk Calculator, which takes into account age, sex, cholesterol numbers, blood pressure, and other factors, a CAC scan can provide clarification.
How the CAC test works
Any plaque in your arteries contains not only cholesterol and other fatty substances but also the mineral calcium. Evaluating the calcium component is critical. X-rays can’t “see” the fatty part of the plaque, but a 10-second CT scan that releases about as much radiation as we are exposed to naturally over six months picks up the calcium deposits. Specifically, it shows the amount of calcium in the coronary arteries—vessels that supply blood to the heart—by taking cross-sectional images of them. The more calcium there is, the more plaque is present that can potentially rupture and cause a clot that leads to a heart attack.
A CAC score of zero means no calcified plaque is present. Guidelines from the American Heart Association and the American College of Cardiology say that someone with a somewhat high LDL cholesterol reading but a CAC score of zero and an intermediate, 10- to 15-year heart disease risk (somewhere between 7.5 and 20 percent, according to the Heart Risk Calculator) can discuss with their doctor the possibility of not starting on a statin but rather rechecking the CAC score in about five years. If the CAC score is somewhere between zero and 100, the risk for heart disease goes up and makes a much greater case for the initiation of statin therapy. If the CAC score is higher than 100, the risk of a cardiovascular event is greater still, and it becomes that much more important to begin taking a statin.
CAC tests can help identify people who have not been taking statins (because their cholesterol is low, for example) but should be (because their CAC score is high), as well as identify those who would seem to require a statin because of their blood cholesterol levels but don’t need to, based on actual plaque accumulation. In research published in the Journal of the American Heart Association in 2020, it was found that one in three people who might be prescribed a statin would be reclassified as not requiring the drug based on CAC results.
Not for everyone
CAC scans are not recommended for people younger than 40 because few people in their 30s and younger have enough calcium deposits in their artery walls to require the initiation of drug therapy to prevent heart disease. It is also not recommended for people who have had a cardiovascular event in the past. They are already considered at high rather than intermediate or low (or borderline) risk. Those whose LDL cholesterol is 190 or higher don’t need the test, either. At that cholesterol level, the American Heart Association says a statin is called for even if the risk calculator says they are at intermediate risk.
In determining whether a statin is right for you, your doctor should review not only your scores on different tests but also your lifestyle, including your diet, your exercise habits, whether you smoke, and your weight. Having a family history of heart disease or diabetes or having a chronic inflammatory condition such as rheumatoid arthritis or psoriasis—all of which increase the risk of a cardiovascular event—may also nudge your doctor in the direction of prescribing a statin even if your CAC score turns out to be on the low side. In other words, it’s not just a numbers game but also a holistic look at how you live and what other medical conditions you have or are predisposed to develop.
BOTTOM LINE: If you have high LDL cholesterol, and if based on your overall health profile your heart disease risk is such that medication would help, you can begin statin therapy right away. Another option, if you are at intermediate risk for heart disease according to the Heart Risk Calculator and are otherwise healthy and also have a healthful lifestyle, is to go for a CAC test and decide about statins in consultation with your physician based on those results. Note that currently, most health insurance companies do not pay for CAC scans, which range in cost from as little as $100 to as much as $500. That’s not an insignificant upfront cost, but for some people the answer it helps provide can be invaluable.
You plug your age, sex, cholesterol numbers, and blood pressure into the Heart Risk Calculator issued by the American College of Cardiology, and it tells you in an instant that you have a 15 percent chance of having a heart attack or stroke within the next 10 years. That puts you at intermediate risk, which is anywhere from a 7.5 percent chance to a 20 percent chance.
Part of what drives up your score is an LDL cholesterol level of 160 mg/dl. It should be under 130, and ideally under 100. Your doctor says it would be a good idea to start taking a statin drug to reduce your blood cholesterol and lower your heart disease risk, but you resist. You have remained at a healthy weight, exercise regularly, don’t smoke, don’t have diabetes, and don’t even have a strong family history of heart disease.
Your physician understands your hesitation and suggests that to get a better indication of your heart disease risk you go for a CAC test. If the score is higher than zero, the case for taking a statin becomes significantly stronger.