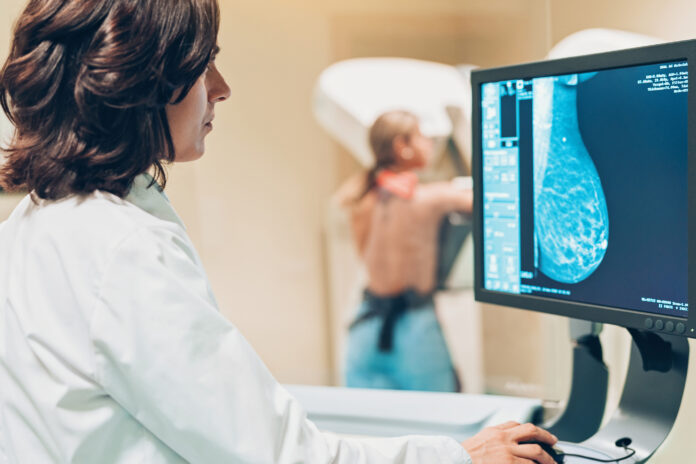
In a major shift, an influential medical panel is now advising that women begin routine mammography screening at age 40—a decade earlier than it previously advised. But some experts feel the revamped guidelines do not go far enough.
The recommendations, from the U.S. Preventive Services Task Force, say that most women should start having mammograms when they turn 40, continuing every other year through age 74. For years, the group had advised a starting age of 50—though women in their 40s were encouraged to talk to their doctors about screening and choose what was best for them. This change in advice is important, in part, because recommendations from the Task Force hold a lot of sway. It’s an independent panel of medical experts that advises the federal government, and its guidelines help determine insurance coverage for cancer screenings.
The update brings the Task Force guidelines more in line with recommendations from other groups, including the American Cancer Society (ACS) and American College of Obstetricians and Gynecologists (ACOG). Those two groups have long set age 40 as the year to start mammography screening (with ACS saying that screening between ages 40 and 44 is “optional”).
But critics charge that the Task Force should have gone further. For example, the guidelines recommend screening every other year, rather than yearly, as some other groups do. The Task Force also offers no specific recommendation, such as additional screening tests, for women with dense breasts, who have an increased risk of breast cancer—which means that insurance may not cover those services.
Here’s a breakdown of what the updated guidelines say, and leave unsaid:
Who’s included?
The guidelines pertain to women at average risk of breast cancer and those with a heightened risk due to dense breasts or a family history of breast cancer. It does not include women with a personal history of breast cancer or prior biopsies with findings of high-risk lesions, or women who are at very high risk because of inherited genetic mutations or who had high-dose radiation therapy to the chest when they were young. Those women should discuss their screening options with their doctor.
Why was the starting age changed?
Back in 2016, when the Task Force last updated its guidelines, it said there wasn’t enough evidence on whether the benefits of screening women in their 40s outweighed the risks. Screening does have downsides, including “false positives” that lead to unnecessary, and sometimes invasive, follow-up testing—not to mention the anxiety those false alarms can cause.
Since then, though, two things have changed: First, the rate of breast cancer among U.S. women in their 40s has been rising, by about 2 percent each year, according to the Task Force. That means there’s now more potential benefit from earlier screening, versus a decade ago. Second, there’s been more research. The Task Force now says there’s strong evidence that mammography screening done every other year starting at age 40 could save 20 percent more lives from breast cancer, compared to the old recommendation.
Why screen every other year?
It’s unclear from studies, the Task Force says, whether annual screening ultimately benefits women’s health any more than biennial screening does. Even though annual screening might catch some cancers earlier, it’s not known whether that would affect the course of a woman’s disease or risk of dying from breast cancer. The Task Force concluded that screening every other year offers a “better balance” of benefits and risks than annual screening.
In contrast, the ACS recommends annual screening up to age 55, and then either continuing every year or switching to every other year. ACOG, meanwhile, calls for screening every one to two years. The differing advice can be confusing; your best bet is to discuss the optimal screening frequency with your doctor.
What if I have dense breasts?
Women with dense breasts (more fibrous or glandular tissue than fat) face a double whammy. In addition to their heightened risk of breast cancer, dense tissue makes it harder to spot a tumor on a mammogram. That’s why doctors often recommend additional screening, with breast ultrasound or MRI. The Task Force said it lacked the evidence to endorse that but urged more research. (For the same reason, the ACS and ACOG don’t recommend supplemental testing, either.) So, this is another case where women need to talk with their doctor about what’s best for them. Be aware that Medicare does not cover supplemental screening for women with dense breasts, and private insurance coverage varies.
What about women older than 74?
Few breast cancer screening studies have included women ages 75 and up. Therefore, as in past recommendations, the Task Force says it cannot offer screening advice—either for or against it—to those women. For their part, the ACS and ACOG mention no upper age limit for mammography screening, and the ACS says women should continue with it as long as they’re in good health and are expected to live at least another 10 years. (Medicare covers annual screenings for this age group, despite the Task Force age limits.)
BOTTOM LINE: While guidelines are coming closer to unity on the starting age for mammography screening, women are still left with some critical questions: How often should I be screened? When should I stop? Do I need supplemental screening, and can I afford it if insurance won’t cover it? Take these questions to your doctor. The most important thing, as mentioned above, is that you have these discussions and figure out the screening plan that’s best for you.