It’s been almost six years since the start of the Covid-19 pandemic, and a lot has changed about the way we view the illness. We now have vaccines and treatments that are effective at preventing severe cases of Covid, and nearly all of us have some immune defenses against SARS-CoV-2, the virus that causes Covid—built up from multiple vaccinations, prior infections, or both.
The face of Covid is changing accordingly. We still experience winter and summer surges in Covid cases, but hospitalizations and deaths from the illness have dropped sharply since 2022. This past winter, the flu sent more Americans to the hospital than Covid did, for the first time since the pandemic began. (That’s due to both a continuing decline in severe Covid cases and a particularly bad flu season.)
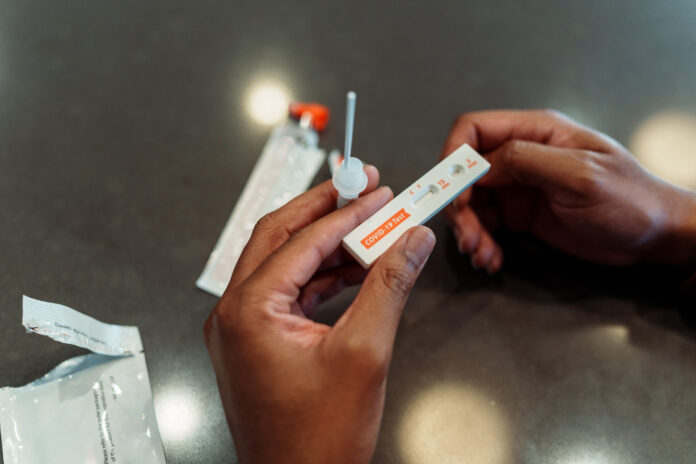
In short, Covid has become an illness that we’re learning to live with, just as we do other respiratory infections. For many people, that may bring up questions about whether they need to keep doing all the things they did during the pandemic—including self-testing for Covid.
Broadly, I think the answer is yes. Since the pandemic began, I’ve had what I strongly suspected was a cold or my standard seasonal allergies, but I still tested for Covid. No one (not even an infectious disease physician) can self-diagnose based on how they feel. Covid can cause symptoms like cough, breathing difficulty, fatigue, and fever, but the symptoms also vary from person to person and can be similar to those of the flu, respiratory syncytial virus (RSV), or the common cold.
It’s true that if you’re sick, you should stay home, regardless of the specific viral cause—for your sake and the sake of others. But it can still be critical to nail down that cause, when possible. And there are now home tests that can detect not only Covid but also influenza A and B (available in the same price range as Covid-only tests).
Although ultimately the decision to test yourself is personal, it’s often the responsible thing to do, and I recommend it for these situations in particular:
- Are you at high risk of becoming severely ill from Covid (or the flu), or around other people who are at high risk? If the answer is yes to either, testing is important. Antiviral medications are available for Covid, including nirmatrelvir/ritonavir (Paxlovid), remdesivir (Veklury), and molnupiravir (Lagevrio)—and for influenza, including oseltamivir (Tamiflu), zanamivir (Relenza), and baloxavir (Xofluza). Those drugs reduce the risk of hospitalization and death, and they can also lower the amount of virus your body “sheds,” as well as the duration of that viral shedding. That, in turn, may reduce the risk of transmitting the virus to someone else. In addition, if you find out you have Covid (or the flu), and not an ordinary cold, you’ll know you need to be particularly careful around high-risk people.
Time matters. To do their job, antiviral medications should be taken early in the course of the illness. So if you would consider taking those drugs, you should self-test as soon as possible after your symptoms begin. Don’t wait until they worsen.
- You may want to test if you know you’ve been exposed to someone with Covid but do not have symptoms. People infected with SARS-CoV-2 can spread the virus for 24 to 48 hours before they develop symptoms, so testing can be useful if you’re concerned about potentially infecting others. The general recommendation is to wait five full days after exposure to someone with Covid to test yourself if you have no symptoms (or to test immediately if you do develop symptoms).
Remember that many people fall into the category of “high risk” for severe Covid or influenza, so there are plenty of circumstances where self-testing is wise. Older age is the strongest risk factor: Adults ages 65 and older account for most Covid and flu hospitalizations and deaths. But the list of risk factors is long, and it includes heart disease, diabetes, kidney disease, pregnancy, and lung conditions like asthma and chronic obstructive pulmonary disease (COPD). In addition, infants younger than six months (who are too young to be vaccinated) are also at increased risk of ending up in the hospital from Covid or the flu, so anyone who spends time around an infant should be particularly cautious when they have respiratory symptoms. In other words, testing is worthwhile in many circumstances.
If you’re looking for resources, the U.S. Food and Drug Administration maintains a list of authorized at-home tests for Covid or Covid/influenza. One important note: Most at-home tests are antigen tests, which are not as good at detecting very small amounts of virus as the tests used by healthcare professionals, called nucleic acid amplification tests, or NAATs (which include PCR tests). So if you get a negative result on an antigen test, you should test again after 48 hours to reduce the chance of a false negative. (While home tests are convenient, you could consider skipping the home approach altogether and heading to a testing center for a NAAT—especially if you’re at high risk.)
Finally, I think home testing is valuable for gauging when it’s safe to return to your usual activities. Symptoms are a helpful guide, to an extent: You should isolate from others until your symptoms markedly improve and you’ve been fever-free for 24 hours (without using fever-reducing medication). But if you’re feeling better and still have a positive result on an at-home Covid test, I recommend keeping up your precautions until you test negative. And even once you’re feeling good and testing negative, I suggest wearing a good mask (N95 or KF94) any time you’re around high-risk individuals, for a total of 10 days after your first symptoms.
While severe cases have been going down over time, Covid killed between 500 and 1,000 Americans each week during its winter peak this year. We should continue to take it seriously and do what we can to keep ourselves and others safe.