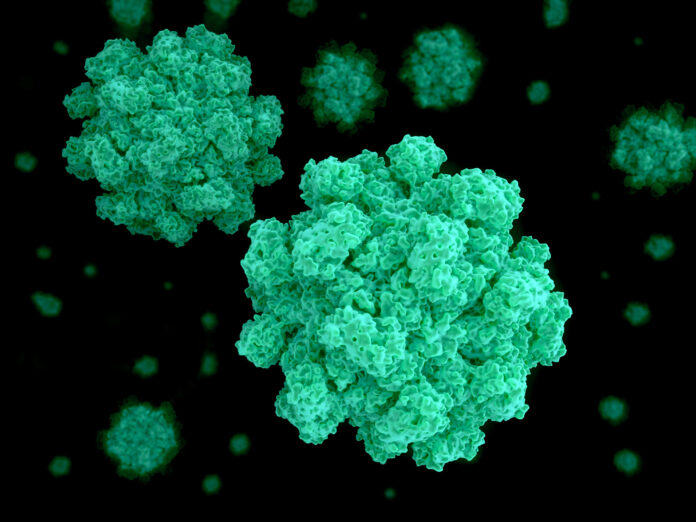
Over the last few months, a lot of people have been suffering from debilitating abdominal pains, nausea, and vomiting that lasts several days. Sometimes they have had diarrhea, too. But no fever. What’s going on? The answer: norovirus, which the CDC reports has been on a steady upswing since last autumn.
The first time I likely encountered norovirus was in the mid-1960s, when I was an undergraduate at UC Berkeley and about a third of the members of my fraternity became ill with vomiting and diarrhea. I dodged the bug, but when I took a friend to the student health center, I saw a line of stricken students stretching down the steps and around the block. They would periodically vomit into the hedge that ran alongside the building.
It was several more years before the pathogen was identified (in 1972) and named for a 1968 occurrence in Norwalk, Ohio, but I was pretty sure the Berkeley students had suffered from an outbreak of norovirus. At a football game the day before, many of them had been eating Gremlins (frozen orange juice in a dixie cup) that had somehow been contaminated with norovirus.
It wouldn’t have taken much: As few as 10 ingested particles of norovirus can cause an infection. What’s more, norovirus can live a long time on surfaces, is insufficiently disabled by many disinfectants, and is stable in acid, which means stomach acid won’t stop it. It can also change its genetic structure on a regular basis, so, like Covid-19, it can evade our immune response; you may develop immunity to one strain, but another may emerge in a few years. Particularly noteworthy is that the virus is undeterred by hand sanitizer, because its capsid, or protein shell, protects it from agents like alcohol that easily damage unencapsulated pathogens like Covid.
These are all reasons norovirus is arguably a perfect human pathogen—from the pathogen’s point of view. Primarily a winter-season, food-borne disease, it’s highly transmissible and very hardy, yet doesn’t usually make people sick enough to go to the doctor or stay inside for an extended period. Instead, infected people remain in circulation, shedding viral particles everywhere they go (like into the Berkeley hedge) for as long as 21 days. Norovirus illnesses are quick, with just one to three days of symptoms, and comparatively minor, as held up against, say, the far more dangerous rotavirus, for which an effective vaccine has been developed. Norovirus, on the other hand, is a real pain, but unless you’re really at the extremes of age or not in good health to start with, it rarely will land you in the hospital. While it can transmit and flourish in the human population, it doesn’t raise its head high enough to draw our attention. Consequently, the scientific community hasn’t focused on it to a degree that has led to its eradication or even treatment.
And yet, norovirus will make victims generally miserable and impact their productivity, even without frequent lethal outcomes. According to the CDC, there are 19 to 21 million cases a year, on average, in the United States, resulting in 900 deaths, mostly among adults ages 65 and older; 109,000 hospitalizations; 465,000 emergency department visits, mostly in young children; and 2,270,000 outpatient clinic visits annually, mostly in young children. Globally, the CDC says one of every five cases of acute gastroenteritis is caused by norovirus; that’s estimated to cause 685 million cases. Annually, norovirus is estimated to cost $60 billion due to healthcare costs and lost productivity. And all these are likely underestimates, since tracking of norovirus statistics is notoriously unreliable.
So what can you do to combat the perfect pathogen? And what’s the best course of action if you do catch it?
Washing your hands with soap and water is the first, best line of attack (don’t rely on hand sanitizer). The reason that works is not that the virus is destroyed like Covid or influenza would be, but because the physical washing process keeps the virus from sticking to the skin. When it comes to food prep, wash your fruits and vegetables. Cook oysters and other shellfish thoroughly to an internal temperature of at least 145°F; noroviruses are able to survive temperatures up to that, and an outbreak linked to raw oysters from Texas in late 2022 was one of the notable recent norovirus events. The CDC advises that anyone who is sick shouldn’t prepare foods or provide care for others until two days after symptoms resolve.
In addition, the CDC says that after someone vomits or has diarrhea, the affected area should be cleaned and disinfected immediately, using gloves and a bleach-based household cleaner or other disinfectant registered as effective against norovirus by the Environmental Protection Agency. The disinfectant should be left on the area for at least five minutes, and then the area should be cleaned again with soap and water.
If you do get infected, the most important thing is to stay hydrated. One of the only ways you can get into real trouble with norovirus is if you don’t replace fluids. Of course, that’s easier said than done if someone’s vomiting. Indeed, older people are more at risk from norovirus because they aren’t able to compensate as well. So be vigilant, wash your hands, and drink up. And maybe skip the Gremlins.