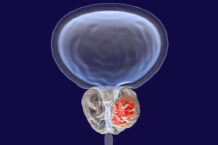
Prostate cancer is the second leading cause of cancer among men in the United States, after non-melanoma skin cancer, as well as a leading cause of death. According to the U.S. Centers for Disease Control and Prevention, more than 250,000 new cases of prostate cancer were reported in 2022, and almost 34,000 men died from the disease in 2023.
For decades, a test for prostate-specific antigen (PSA) has played a key role in screening for prostate cancer. Although an elevated PSA level can indicate the presence of cancer, it can also be triggered by unrelated factors. Because of these and other uncertainties, screening and treatment guidelines have often generated significant controversy.
It is generally recommended that men receive a baseline PSA test between the ages of 45 and 50, with the timing based on individual risk factors and a discussion with their healthcare providers. They should then receive regular screening through the age of 69. Standard practice is to stop PSA screening at around age 70 for men who have been screened regularly. (For men who receive their first PSA at 70, the calculations about future screening are a bit different.)
Prostate cancer is very common in older men, but it most often grows slowly, so most men who have it will die of something else. Given that, the news in May that former President Joe Biden was suffering from an “aggressive” form of prostate cancer, and that it had already metastasized into the bone, seemed to come out of nowhere. The Wellness Letter spoke with Dr. Peter Carroll, an expert in prostate cancer and a professor of urology at UC San Francisco, about Biden’s diagnosis, current approaches to assessment and treatment, and related issues.
Wellness Letter: Many people were surprised at the news about President Biden. Can you provide some context on the situation and how this might happen?
Peter Carroll: Decisions on prostate cancer screening are made in consultation with patients. We discuss the risks and benefits based on their age and other circumstances. We don’t know about the conversation President Biden and his doctor had about a decade ago when he was in his early 70s and last had a PSA test. I think the story goes back to that last PSA test, and his PSA history before that. We don’t know what those were.
Maybe in 2014 his PSA was very low, and it had been low for many years. That would have meant his future risks were low and that the decision not to keep screening after that would have been reasonable. But even if someone were getting screened every year, they could have a fast-growing cancer like his, without having any symptoms. It’s not common, but we do see it.
We just don’t know the full story. There is also the secondary issue of whether there are different considerations for a person in his position compared to those who aren’t leading the country. Maybe the standards for screening should be higher for him than for you and me and others who don’t have that job, which demands a very high degree of physical and mental vigor.
WL: What is the current thinking on the value of PSA testing?
PC: I think PSA screening is important. A baseline PSA at age 45 is very predictive of the future risk of prostate cancer and the future risk of developing metastatic disease. With a baseline PSA, along with family history and background, you can determine whether someone needs to be rescreened every year, or two years, or perhaps four years.
However, while PSA screening predicts risk, it is not specific for cancer. If you screen 1,000 men in the U.S., about 250 will have an elevated PSA. If you biopsy all those men, you’ll find that about half don’t have cancer. They just have benign prostate enlargement. Men with an enlarged prostate, which is common as they get older, often have higher PSA levels.
WL: Is the overall approach to prostate cancer and PSA screening different than previously?
PC: Definitely. I’ve been doing this a long time, and there’s been a sea change in how we look at prostate cancer, how we assess it, and how we treat it. PSA screening really gained traction in the mid-1990s. At that time, you would screen all men, you’d identify the disease, and you’d treat all of them. And the data have shown that PSA screening does save lives.
But what’s also become clear over time is that there’s a real issue with over-detection and over-treatment. Over-detection means detecting a cancer that would not be a problem for you over your lifetime, if undetected. Over-treatment is treating that patient’s cancer, so they might experience side effects from treatment but with no benefit.
WL: With prostate cancer, can you know whether it is one that does or doesn’t need to be treated?
PC: I think now you can, and UCSF has been a leader in this. We have one of the largest cohorts of men on active surveillance [i.e., being followed for a period of time without treatment unless the cancer progresses] in the world. Many, many men get diagnosed with low-grade, low-volume cancers. We’ve documented the safety of active surveillance in these cases. For example, the risk of metastases with these low-grade cancers is very low—about 1 percent over 10 years.
Over that time, about a third of the men will get treated because we see some changes in the cancer. But if you can delay that treatment for five or 10 or 15 years with active surveillance, that’s a win—the patients haven’t suffered any side effects from treatment in the meantime. Men and their families need to make decisions based on the best information currently available. Frequently they don’t get this information.
WL: So what is the approach when someone has an elevated PSA?
PC: We’ve now developed some secondary tests that can tell us the likelihood that someone with an elevated PSA has clinically significant disease—not just any cancer, but something that you might want or need to treat. We have a host of options—serum and urine tests, prostate MRIs that tell us the risk of having a clinically significant prostate cancer, and genomic profiling, for instance. Based on that information, we might decide to go ahead with a biopsy.
In recent years, thanks to these options, we’ve been able to decrease biopsy rates at UCSF by at least 30 to 40 percent. In other words, we’re doing biopsies very selectively now. And if a biopsy is necessary, an MRI scan can help ensure a more targeted biopsy.
Before doing a biopsy, however, I always tell men about the risk of over-detection of prostate cancer. I tell them, “Look, you have to understand that I may identify a cancer and then I’m going to tell you that it does not need to be treated.” And I give them the data. The time to tell men about this is before the biopsy is done, not after, because many men will hear “cancer” and they equate it with having a lethal disease.
WL: How do you decide when active surveillance is the best strategy and when it is necessary to begin treatment?
PC: If you look at men with early-stage, non-metastatic disease, the first question you always ask is, do they need treatment at all? So again, based on cancer grade, volume, genomics, MRI imaging, you can select those patients who may not need any initial treatment at all. That’s when we do surveillance.
In these cases, we’ve also been able to minimize the surveillance regimen. It used to be that men would have to get a follow-up biopsy every year. We found we can now predict the likelihood of progression so we can tailor the scheme to the needs of individual patients and reduce the number of follow-up biopsies.
We have a range of options for treatment. The decision on when and how to treat is ultimately based on three criteria. One is the nature of the cancer itself. Then you look at the age and health of the patient, whether they have any comorbidities—heart or lung problems, for example—and lastly, the preferences of the patient. It’s important to spell out clearly the most common side effects of treatment—problems with bladder, bowel, and sexual function.
WL: Getting back to Biden, what is standard treatment in cases like his, and what is the prognosis?
PC: I think the treatment would be very similar at all major medical centers, like UCSF, Sloan Kettering, Johns Hopkins, and others. You would need to know some other details, but the most common treatment is called augmented hormonal therapy, which involves reducing serum testosterone levels. Almost all prostate cancers, at least initially, are “androgen dependent,” meaning they’re driven by the level of testosterone. Overall, the long-term outcomes for men with metastatic disease are far better now than they were 20 years ago.