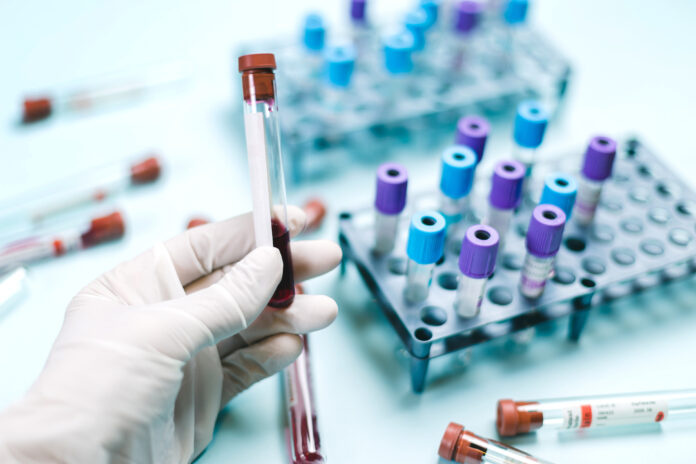
In the past couple of years, an increasing number of articles in mainstream news publications have touted an emerging technology with the potential to revolutionize cancer treatment: multi-cancer early detection tests, also known as liquid biopsies. Unlike invasive tissue biopsies that can detect specific kinds of cancer, liquid biopsies are designed to test blood samples for DNA molecules associated with dozens of cancers.
For further information, the Wellness Letter turned to Jeffrey L. Wolf, M.D., a hematologist/oncologist at the University of California, San Francisco, and a member of our editorial board. Dr. Wolf is an expert in cancers of the blood and bone marrow, and in particular myeloma. He obtained his medical degree from the University of Illinois College of Medicine at Chicago followed by his residency at UC San Diego, a fellowship in hematology and oncology at UCSF, and a rotation in bone marrow transplantation at the Fred Hutchinson Cancer Research Center in Seattle.
We asked Dr. Wolf to explain how these tests work and to provide some guidance on their current role in patient care, if any. (During the conversation, he referred to results on how the tests performed on a variety of cancers from a study in the Annals of Oncology in 2021.)
Wellness Letter: What is the background on these multi-cancer early detection tests?
Dr. Jeffrey Wolf: A dozen or so years ago, the whole concept of a liquid biopsy was being discussed and seemed to offer hope that it could identify cancers earlier than other techniques. The tests used in these early investigations produced too many false positives, however, meaning that they suggested cancer when there was none there. And that means you would end up with a lot of unnecessary and expensive procedures, which would create a great deal of anxiety in patients. Therefore, nothing much happened in the field for a number of years. And then several new technologies were developed. One company, Grail, has become the leader in this whole area. They started working with a technology that could identify some cancers using methylated DNA [DNA to which is attached a methyl group consisting of one carbon and three hydrogen atoms]. They and others are pushing these assays now.
WL: How accurate is this new generation of tests?
JW: As opposed to the earlier sets of tests, which had too many false positives, the specificity of the new tests turns out to be quite good. The higher the specificity, the greater the likelihood that a positive test is truly detecting cancer and the lower the likelihood of false positives. The problem is then on the sensitivity side—that is, possibly missing some cases of cancer, especially in early stages, when the cancer is small and more easily treated. What’s the point or advantage in detecting cancer when it’s already metastatic and you can identify it in other ways? If the tests have low sensitivity, they may not result in false positives, but they might miss early disease. That could reassure people that they don’t have cancer when they actually do.
WL: And that raises the question of whether these tests are worth the costs.
JW: Right. My concern is that a lot of money will be spent by a lot of people and the tests still might miss cancers. The question then becomes how often do you have to do the tests to pick up earlier cancers. Presumably you’d have to do it every year so you can pick up something in the earlier stages. You’re just not going to do it once in your lifetime, right? And they’re not cheap. So if there are 100 million people in the U.S. over age 65, do all of them get these tests every year? What is the cost of that? The current list price is $949. So, if you do that every year, who pays? Medicare? Or do you pay out of pocket, so rich people get it and poor people don’t? Those are the questions that have to be asked and answered.
WL: How well do the tests perform with particular cancers?
JW: In the case of the test developed by Grail, the company claims it detects 50 different types of cancer. But this paper [from the Annals of Oncology] includes just 12 cancer types. You’ll see that several aren’t even represented here, like breast cancer. Could that be because the test doesn’t do well with breast cancer, which is the most common cancer in women besides skin cancer? And there’s no prostate cancer here. And part of the reason is you can usually pick up prostate cancer early with a PSA test, so you don’t need this test to pick that up. The point is that if you’re looking for a specific cancer, you may have better tests.
And for anal cancer, to pick it up at stage one, the test is only 75 percent sensitive. That’s going to miss a quarter of the anal cancers when they’re in stage one. Maybe the test would start picking them up when they’re in stage two, but the patient would probably already have symptoms by then. For lung cancer, it’s 22 percent sensitive in stage one. For ovarian cancer, 50 percent. For stomach cancer, only 17 percent.
WL: The test is designed for people without any symptoms, right?
JW: Yes. It is a general screening test to supposedly pick up any of these cancers that you might have, but you wouldn’t know it because you’re not experiencing any symptoms. It would not be used for screening anybody if they already have particular symptoms. If somebody is symptomatic, then you order tests that are specific for the symptoms. So, if somebody has blood in their stool, for example, you look for anal or rectal or colon cancer, but you don’t test for breast cancer.
An ideal test would pick up all cancers when they’re stage one, and you’d be able to tell specifically that we just picked up a signal for a bladder cancer, for example, and then you investigate that directly and you find it when it’s still early stage, so you can resect it [surgically remove the cancerous tissue]. But the current version is not generally good at identifying stage one or sometimes not even at stage two cancers. Tests like this would be useful with a much higher sensitivity in stage one and much lower price point.
WL: And what about people with a family history of cancer?
JW: For people with family members who have had a certain kind of cancer, you might just look for that one cancer. We’ve got ways of testing for myeloma, we have ways of testing for pancreatic cancer, we have ways of testing for ovarian cancer, so you can be more specific about what you’re looking for. And even with the Grail test, older women should still be getting mammograms and men should be getting PSA testing, and so on. Because, again, this just picks up certain cancers, but often late.
So, the message is this—these tests might have a role, but they can’t be used alone. There are other questions too. Should everyone have this done, or just some people? How often should it be done? We don’t know.
WL: We also don’t know if the tests actually have any impact on catching cancers and improving long-term outcomes, right?
JW: That’s right. These tests may miss cancers, but the liquid biopsy approach appeals to people and might be widely used without an understanding of the limitations. Even if the data show that it doesn’t make a difference across a population, it might make a difference for one particular person. Someone might do this test and in their individual case, it could pick up early-stage bladder cancer, and that’s what you hear about on the news, right? But even if you spend $1,000 out of your pocket every year for this test, you still might not pick up early pancreatic cancer, early breast cancer, or other cancers in the early stages. That’s why testing can’t be recommended as an intervention on its own at this point. It is really just a complement to existing screening.