The Montreal Cognitive Assessment (MoCA) first made headlines in 2018 when President Donald Trump, during his first term at age 71, was reported to have received a perfect score on the test. You may recall him recounting about how he was able to repeat all five words presented to him—person, woman, man, camera, TV—and remember them a little bit later.
In a redo of the test in his current term this past April, Trump, at nearly 79 years of age, once more reported that he attained a perfect score—calling the test an “IQ test,” though in fact, it was not assessing intelligence but rather screening for dementia.
Supporters have claimed the president’s performance on the test confirms his mental acuity; critics say the screenings prove nothing about his judgment or fitness to be president. Wherever you stand on the political spectrum, however, you may be interested in knowing more about MoCA.
This routine screening test is widely used by doctors in the U.S. to screen for cognitive impairment in older adults. Although MoCA isn’t intended to prove or disprove definitively whether someone is experiencing problems with thinking or memory, it can be a helpful tool when utilized as part of an overall assessment by doctors or other healthcare professionals trained to diagnose cognitive problems.
MoCA screens for all levels of cognitive impairment, including mild cognitive impairment (MCI). People with MCI have memory or thinking problems that aren’t serious enough to interfere with everyday living. MCI can be a precursor to Alzheimer’s disease or other kinds of dementia, but it doesn’t always lead to dementia, and in some people, MCI can revert to normal cognition.
It’s important to note that, contrary to Trump’s claims or what he may have implied, MoCA does not specifically evaluate or reflect one’s intelligence. To assess IQ, more comprehensive testing is needed, and the standard test for that is the Wechsler Adult Intelligence Scale (WAIS). The Wechsler Intelligence Scale for Children (WISC) is for children ages six through 17.
How MoCA works
MoCA is a 10-minute test that assesses a range of cognitive skills, including attention, concentration, executive functions, memory, language and verbal fluency, calculation ability, conceptual thinking, and visuoconstructive skills.
There are multiple forms of MoCA to avoid a “learning effect” if the test is given multiple times to the same person. The tasks to perform may include:
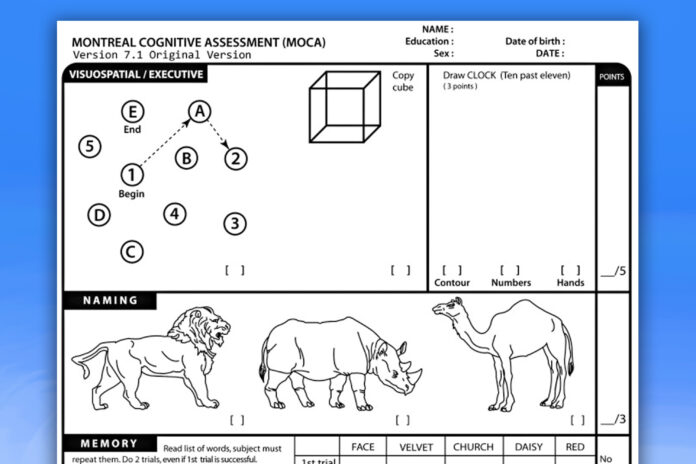
- Drawing a line that alternates between numbers and letters of the alphabet printed on a page, in ascending order (1-A-2-B-3-C-4-D-5-E)
- Copying a drawing of a three-dimensional cube as accurately as possible
- Drawing a clock showing a certain time (10 past 11), without looking at your watch
- Naming three animals presented in drawings (a lion, a rhinoceros, a camel, for example)
- Repeating and later (at the end of the test) recalling a list of five words (face, velvet, church, daisy, red, for example) in any order
- Repeating a list of five numbers in the same order, presented verbally by the test administrator, and then repeating a second list of three numbers backwards
- Repeating two sentences verbatim
- Counting back from 100 by sevens
- Naming as many words as possible that begin with the letter “F” in one minute (naming 11 or more gets a top score)
- Categorizing pairs of words (that is, explaining what each pair has in common), such as banana and orange or train and bicycle
The test also asks questions about orientation (what is today’s date and where are you now?). A perfect score is 30, but a score of 26 or above is considered normal. Lower scores are associated with possible cognitive impairment. Higher scores do not, however, rule out the possibility of subtler (yet still meaningful) cognitive deficits that might be detected through more comprehensive neuropsychological testing.
Certain factors may interfere with screening test results. For example, scores may be affected by a patient’s education level, age, language ability, or the effects of medication they may be using at the time of the test. A patient may also score low on this mental status test because of such factors as fatigue, sleepiness, lack of engagement, anxiety or depression, a distracting environment, or ongoing pain or discomfort.
How accurate is MoCA? According to a 2021 Cochrane Collaboration review, it detected dementia in 94 percent of people with the condition, when a cutoff score of less than 26 was used. But it also had a high rate of false positives, meaning that many people without dementia also scored below normal.
Although many doctors rely on screening tests such as MoCA, routine screening of older adults for cognitive impairment is not recommended. In its most recent report, published in JAMA in 2020, the U.S. Preventive Services Task Force—a federal advisory panel of medical experts that evaluates and makes recommendations about preventive healthcare—concluded that there is insufficient evidence to recommend in favor of or against routine screening. That is, the risk of harm from the screening may not outweigh the benefits for asymptomatic people. “More research is needed,” the Task Force concluded.
Just one of many screening tools
Mental status screening tests such as MoCA certainly have a place in identifying cognitive impairment and memory loss associated with dementia—in people who are having mental difficulties (as opposed to screening those not showing any signs of loss). However, organizations such as the Alzheimer’s Association recommend that doctors do a full medical workup because no single test can accurately diagnose dementia.
A full workup includes questions about medical history and current health conditions; a physical exam; a medication review; a discussion about mood, diet, and alcohol use; and a neurological exam, which evaluates coordination, balance, reflexes, mental status, and sensory and motor skills. Laboratory testing or brain imaging may also be recommended before a diagnosis is made.
Cognitive changes in older people aren’t always the result of dementia; other common causes include certain prescription drugs, vitamin deficiencies, or medical conditions such as depression, thyroid disease, anemia, diabetes, infection, and diseases of the kidney, liver, or heart.
A cognitive assessment should also include a discussion with family members, who can provide context about a person’s memory or behavior. Knowing whether a person’s memory or judgment has worsened over time is crucial for a doctor trying to diagnose any kind of cognitive decline.
BOTTOM LINE: Despite its reemergence into the spotlight, the MoCA and other mental status scales are just a starting point, offering clues—not verdicts—about memory and thinking. Compared with comprehensive neuropsychological testing, these mini screenings are not as well standardized or validated. True cognitive assessment requires a full medical workup and context from those who know the person best. And that involves far more than a 10-minute test of repeating words, naming animals, and drawing clocks. If you or a loved one is experiencing cognitive issues beyond those “senior moments,” it’s a good idea to consult a primary care doctor, who may recommend further evaluation with a neurologist or other cognitive specialist.
Spouses, partners, or other close relatives or friends are often the first to spot signs of cognitive decline in a loved one. It may be an adult child who first notices a parent not acting as usual. The following signs might be a hint that someone needs to be assessed:
- Losing or misplacing things such as keys more often than in the past
- Struggling to think of the right words to express a thought or identify an object
- Forgetting to keep appointments
- Forgetting recent conversations or events
- A decline in thinking skills, such as those involving time management or decision making
- Changes in the ability to move
- Feeling disoriented or getting lost in familiar places