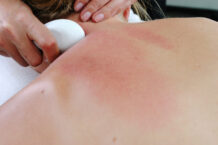
Chronic pain is a serious problem in the United States and is among the most common reasons that people seek medical care. In 2023, according to statistics from the CDC, about 24 percent of Americans reported having chronic pain in the previous three months. Women were slightly more likely to be affected than men.
Chronic pain—which comes in many forms, from back pain, arthritic joint pain, and headaches to neuropathic pain and fibromyalgia—is also increasingly common as people age. Among those ages 18 to 29, about 12 percent reported experiencing it, compared to 36 percent among those 65 and older.
What leads to chronic pain? And what can we do about it? The Wellness Letter spoke with Sean Mackey, MD, PhD, a professor of anesthesiology and pain medicine at Stanford University School of Medicine, about the origins of pain, how our understanding has changed over the centuries, and strategies for managing it.
Wellness Letter: We all know what pain feels like, but why does it happen?
Sean Mackey: The existence of pain goes back to single-celled organisms millions and millions of years ago. Pain and reward, or pleasure, are the two basic drivers that keep organisms alive. We are attracted to and rewarded by oxygen, food, sex, and safety, for example, while pain is a danger signal. It is our harm alarm, and it helps protect us.
WL: How has our understanding of pain changed over the years?
SM: In the 17th century, René Descartes created a mechanistic foundation for pain. He viewed the mind as a passive receptacle for the signals coming in from the body. He assumed these signals or inputs would be experienced pretty much the same by everybody. That idea of a linear, direct relationship between the extent of injury and the amount of pain that people experience has persisted.
That idea of pain is still with us today. But in the last few decades, research has shown that this is all wrong. There are in fact tremendous individual differences and variability in how people experience pain for a given injury or stimulus.
WL: So, for example, an injection might not bother one person at all, but someone else might find the same injection very painful?
SM: Exactly. When I teach a medical school class on pain, I have students put their hand in a circulating ice water bath for 15 seconds, and then they pull their arm out and score the pain from zero to 10. And some say, “Nah, that wasn’t painful at all. I give it a zero.” Some give it a two. Some say four, all the way up to people saying, “My god, that was the most incredibly painful thing I’ve ever experienced!”
The point is to teach our fledgling doctors that pain is very individual. And we have to take care not to project our own experiences of pain onto other people.
WL: Do people often think there’s one thing that can be pointed to as causing their pain?
SM: With pain, people tend to have the mindset that there’s got to be something physical that’s directly tied to that experience. It becomes a problem when you don’t have that obvious direct physical connection. And this is part of the broad problem we have with chronic pain. We don’t have a way of directly seeing it.
For example, you have pain conditions like fibromyalgia, which affects millions of people, mostly women. They have been stigmatized and called histrionic housewives and told they’re somaticizing, that they’ve got a psychological illness.
WL: But if you can’t identify a specific mechanistic cause, or a single mechanistic cause, then what is generating or perpetuating it?
SM: That’s an area of focused research in our lab and many others. We believe that there are multiple factors that can perpetuate or amplify pain. There can be continued peripheral signals being sent to the central nervous system that are driving the pain. There can be alterations in the brain and the spinal cord that can magnify the pain and cause it to persist, even in the absence of something wrong in the periphery.
WL: How much of a current problem is opioid use among people in chronic pain?
SM: The current wave of the opioid crisis is not being driven by opioids prescribed by physicians but by illicit fentanyl. The vast majority of people with chronic pain are not taking opioids. The vast majority of people with chronic pain who are taking opioids are taking them responsibly. Only a small percentage of people really run into problems with prescribed opioids, and I’m always careful not to conflate the treatment of chronic pain with opioids.
For a period of time, doctors were clearly prescribing too many opioids and were not well trained on how to use them—how to put people on them, how to take people off of them. And that caused a lot of problems. But prescription opioids have dropped off dramatically.
WL: Is chronic pain ever fully curable?
SM: Every once in a while, we can identify a particular lesion [a damaged section of tissue] or a specific problem, and we can cure somebody. Those cases are great, incredible. We all remember them. But I rarely talk to patients about cures of their chronic pain, because I don’t want to set unrealistic expectations.
We typically focus on helping people find ways to get control of the pain, to reduce the impact it has on their lives. Most people realize that they’re going to be dealing with aches and pains as they age, but they want their quality of life back. They want control of their life back; they want to get back to a higher level of functioning. That’s what we work toward giving people.
WL: How do you do that? What does pain management consist of?
SM: In general, we have six categories of therapies that have shown some benefit for chronic pain. First, we’ve got at least 200 medications with some pain-relieving properties. Of those, only 20 are opioids. Second, we have some minimally invasive surgeries and interventional procedures, such as nerve blocks and epidural steroids. Third, we have mind-body or psychological approaches, which are typically based on cognitive behavioral therapy and mindfulness techniques.
Fourth, we have physical and rehabilitative approaches, typically variants of physical and occupational therapy. Fifth, we have complementary or alternative medicine approaches, like over-the-counter nutraceuticals and acupuncture. And sixth, perhaps the most important one, is self-empowerment, and that involves self-education and learning about pain.
Those six pillars are the basis for everything that we do in pain management. For particularly complex problems, we find it’s best to bundle them together. The challenge that we have in our field is that we don’t have this precision approach where we can take a particular person with their particular chronic pain problem and say, “This is exactly the treatment that’s going to fix it.”
WL: You mentioned that self-empowerment might be the most important pillar. Can you elaborate?
SM: Our research has shown that one of the factors most associated with increased pain and poorer outcomes is low health education. By that, I don’t mean education in general, but rather education about your health condition. Self-empowerment means increasing your health education to better understand your condition and how to treat it.
Self-empowerment shifts people from passive recipients of care to active partners by breaking the cycle of helplessness through education about pain mechanisms and treatment options. It also enables personalized solutions, since chronic pain often lacks a single cause and requires tailored combinations of therapies. Self-empowerment also builds psychological resilience by reducing catastrophizing, improving coping, and creating sustainable habits through goal-setting and activity pacing.