Over the years, I’ve noticed people with the skin condition vitiligo. But as a middle-aged man, I was surprised when I recently developed it myself on my hands, since I thought it started at a younger age. What causes the loss of skin pigment, what are the best treatment options, and is there anything I can do to stop it from progressing?
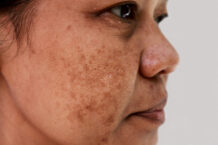
You’re right that this autoimmune skin condition often appears earlier in life, usually before age 30, but it can show up at any age. In vitiligo, your immune system mistakes melanocytes (the cells that produce the skin-darkening pigment melanin) for foreign invaders and attacks and destroys them. The loss of these cells creates patches of lighter-colored skin in places like the hands, feet, arms, face, neck, and genitals.
Interestingly, in generalized (aka nonsegmental) vitiligo—the most common type and the focus of this article—the depigmentation typically occurs all over, often on both sides of the body in symmetrical fashion, and usually worsens over time. (In contrast, segmental vitiligo tends to develop rapidly on one side of the body and then stabilize after six to 12 months.)
Although vitiligo is estimated to affect only 0.5 to 2 percent of the population worldwide, celebrities like Michael Jackson and model/advocate Winnie Harlow have brought it into the public spotlight. And while it strikes all racial and ethnic groups equally, it’s more visible on darker skin.
What causes the loss of pigment cells involves a complex interplay of genes and environmental triggers. Researchers have identified more than 30 gene variants that increase susceptibility to vitiligo. Then, some physical or environmental stressor—such as trauma or injury to the skin, ultraviolet (UV) radiation resulting in a sunburn, or chemical exposure—sets the destruction of melanocytes in motion. Psychological stress may also play a role. People with vitiligo may have other autoimmune conditions as well, such as Graves’ disease, alopecia areata, rheumatoid arthritis, pernicious anemia, or psoriasis.
How much of the skin is affected varies from person to person. Some people develop only a few small patches. Others have large areas of depigmentation. If vitiligo is in a place where hair grows, like the scalp, the hair can also lose its pigment and turn silver or white. Treatment is aimed at stopping the damage to melanocytes, evening out skin tone, or restoring pigment when possible. Your dermatologist might use a special light to better delineate the extent of your vitiligo and to monitor treatment.
Topical corticosteroids are considered the first medication for vitiligo that is limited in scope, but these anti-inflammatory medicines are meant only for short-term use (just a few months) because of the risk for side effects like skin thinning, excess hair growth, and rashes. Adding the medicine calcipotriene may repigment the skin better and faster than corticosteroids alone (but is not effective on its own).
Tacrolimus ointment and pimecrolimus cream are alternatives to corticosteroids for vitiligo on the face and neck and are safer to use for longer periods of time. Ruxolitinib (Opzelura) is a newer topical treatment, approved by the FDA to restore lost skin color in nonsegmental vitiligo. A last option if you have a lot of vitiligo in visible areas is to depigment the remaining color from the skin using a variety of drugs so that it matches lighter areas.
Another treatment is phototherapy, which exposes your skin to UV light to restore pigmentation. It’s an option when vitiligo covers a large area or if topical medications haven’t worked well enough, but it can take several sessions to see improvement—and few dermatology offices offer it anymore due to space and time limitations. It can also be done at home. Laser treatment is an alternative to phototherapy for treating small areas of pigment loss.
Surgery is considered only after other treatments have failed to produce improvement. It involves grafting a section of healthy pigmented skin or skin cells onto affected areas.
Researchers have investigated whether antioxidants like vitamin C, vitamin E, and ginkgo biloba might improve skin repigmentation, but studies haven’t been well designed enough to confirm a benefit for these or other supplements. According to a position statement from the International Vitiligo Task Force, however, there is some evidence that antioxidant extracts from Polypodium leucotomos (a fern species) and gliadin-protected superoxide dismutase (SOD), in combination with phototherapy, might boost improvement.
Sun protection is essential with vitiligo. The pigment melanin normally shields the skin from harmful UV rays. Without it, your skin is more likely to burn, so you should avoid the sun when possible and wear sunscreen and sun-protective clothing while you’re outside.
Vitiligo progresses differently for each person. For those who develop it at a young age, more areas of skin are often involved and progression tends to be faster. Treatment should stop pigment loss, and possibly restore color to the skin, but the condition often comes back. To keep seeing results you’ll need to stay on a maintenance medication long-term. Your doctor will schedule follow-up visits about once every three to six months to see how well your skin is responding, and make treatment adjustments, if needed.
A final note: Vitiligo isn’t life-threatening—but it’s not just a “cosmetic issue” either. The high visibility of the skin patches can cause significant distress and low self-esteem. People with vitiligo are often stigmatized and bullied, and they are more likely to develop depression than those without it. Until treatment starts to work, you can camouflage areas of lost pigment using makeup, self-tanner, or skin dyes. Seeing a therapist or other mental health professional can help you manage any depression, anxiety, or other emotional stress related to vitiligo.