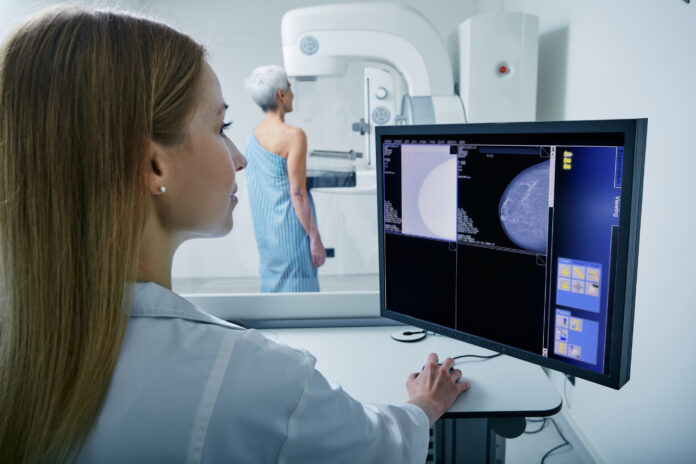
No woman wants to get that dreaded call saying her routine screening mammogram has abnormal, suspicious, or incomplete findings. But if that happens to you, there’s no reason to panic. In most cases, the results are actually benign but may require additional testing and follow-up. Dense breast tissue, which is present in about 50 percent of women, is one scenario that can make imaging difficult and may require more images to be done. Another common reason is a finding of calcifications in the breast, which increase with age and appear in upwards of 80 percent of mammograms.
These tiny deposits of calcium within breast tissue are too small to be felt and frequently show up first on a mammogram (the calcium absorbs the X-rays, making them easy to see). Calcifications aren’t related to the calcium in your diet—rather, they are considered a marker for other things happening in the breast, such as injuries or infections, inflammation, cysts, prior radiation therapy, calcium buildup inside blood vessels, and tumors (both benign and malignant).
All of these processes can cause abnormal cells to grow inside the breast tissue. When these cells die and the body cannot clear them away, the cells harden and calcium deposits form. However, calcifications themselves are not cancerous and cannot become so.
“Calcifications seen are not a direct marker for breast cancer,” says Rita Kwan-Feinberg, MD, a surgeon at Sutter East Bay Physicians Medical Group in Oakland, California, and a member of our editorial board. “Rather, this is a radiographic finding and, depending on characteristics, may indicate the presence of abnormal cells.”
Sizing them up
Calcifications are classified into two groups largely based on their size, and it’s not uncommon to have a mix of both types.
- Macrocalcifications are greater than 0.5 mm and typically appear as well-defined lines or dots. They are more commonly seen in older women, particularly after age 50, and they are usually caused by aging arteries in the breast, prior injuries, or inflammation. These larger calcifications are almost never associated with cancer, and they usually don’t require a follow-up biopsy.
- Microcalcifications, as the name suggests, are smaller—less than 0.5 mm. They appear as tiny flecks, like small grains of salt. When they are seen on a mammogram, they’re more concerning than macrocalcifications, but they are also far from a definite sign that cancer is present. A large observational study in the International Journal of Cancer in 2021 found that microcalcifications became more common with increasing age. And they were most common in women with dense breast tissue, those with risk factors for breast cancer, and those who have had more than two children or breastfed for more than one year.
Location, location, location
In addition to size, it’s the location, shape, and pattern of the calcifications that help determine whether follow-up testing is warranted.
As a general rule, calcifications are likely to be associated with a benign process (with no biopsy needed) if they are larger than 0.5 mm (macrocalcifications), have defined edges and standard shapes, and are not concentrated in one area. For example, many women over the age of 50 have macrocalcifications that appear as well-defined spheres with a transparent center. These are usually due to dead fat cells (fat necrosis) or cysts that have calcified. Even larger macrocalcifications (referred to as “popcorn-like”) are often the result of a benign breast tumor such as a fibroadenoma.
Some features of calcifications that are more likely to suggest cancer include being smaller than 0.5 mm (microcalcifications), varying in shape and size (often called “pleomorphic calcifications”), and being clustered in one location. They may suggest the presence of ductal carcinoma in situ (DCIS), a type of early cancer that stays in the duct, as well as other types of cancer.
Next steps
Although calcifications are not—and will not turn into—cancer, they can signal that abnormal cell changes are occurring in the breast, and it’s important to find out why. Additional follow-up could involve a diagnostic mammogram, which utilizes spot compression and magnification of the affected area. Ultrasounds don’t usually show calcifications, and MRIs never do, but adding these imaging tests may help identify other changes in breast tissue that could suggest cancer.
If your mammogram shows signs of calcifications, the radiologist will classify them in one of three ways:
- Clearly benign: No further testing is required, and you’ll continue to follow your regular mammography schedule.
- Likely benign: You may be asked to come back for another mammogram in six months.
- Suspicious (either somewhat or very): You will need additional testing, often a needle biopsy, which takes a tiny piece of tissue from the affected area to look for signs of cancer. (Even if your doctor decides that a biopsy is needed, a large majority of those biopsies show a benign result.)
A benign finding in all of these scenarios means that your doctor will likely recommend another mammogram after a set time to check for any changes in the number or size of the calcifications (and, as is always the case when possible, all your future mammograms will be compared to your past scans). If the needle biopsy does show signs of atypical cells, however, you may need a surgical biopsy, which samples a larger amount of tissue.
BOTTOM LINE: Calcifications are not cancer, and they can’t turn into cancer. It’s important to keep that in mind, as a call saying that your mammogram requires follow-up can be very scary. Nevertheless, these small white spots can be an early warning sign that something is going on inside the breast tissue—most often a harmless process, but sometimes an important indicator that early intervention is needed. This is why regular mammograms are so important.
Different organizations vary in their screening recommendations. The American Cancer Society recommends that women at average risk for breast cancer begin annual mammograms between ages 40 and 44 and continue through age 54. Starting at age 55, women who continue to be at average risk can choose whether to continue with annual mammograms or switch to every other year. Screenings should continue as long as a woman is in good health and has a life expectancy of at least 10 more years.
The U.S. Preventive Services Task Force’s new guidelines (as of April, 2024) suggest that all women begin mammograms at age 40 and continue every other year until age 74. The American College of Radiology recommends beginning mammograms at age 40 for women at average risk, with earlier and more intense screening for women at higher risk.
These varying recommendations underscore why it’s crucial to go over your family history and other risk factors with your doctor to come up with an individualized screening schedule that makes sense for you.