I’ve been getting regular skin exams from my doctor but read that there’s no good evidence they help prevent skin cancer outcomes. Is there any reason for me to continue to have them?
You’re likely referring to the latest recommendation from the U.S. Preventive Services Task Force, which was released in April. Consistent with its 2016 report, it concluded overall that “the current evidence is insufficient to assess the balance of benefits and harms of visual skin examination by a clinician to screen for skin cancer in adolescents and adults.” But that doesn’t necessarily mean you should stop being screened.
The Task Force is an independent panel of medical experts that makes evidence-based recommendations in such areas as screening, counseling, and preventive medication after reviewing the most up-to-date research and weighing the balance of benefits versus harms for any given preventive care service. The skin cancer screening update is based on a systematic review of 20 studies that, for instance, showed no observable melanoma mortality benefit from widescale skin cancer screening. And when benefits were seen in some studies, they became less significant over time and when other factors were adjusted for.
With that said, it’s important to emphasize up front that the Task Force did not make any recommendations for or against routine skin cancer screening because it found the evidence to be insufficient either way. That is, the panel gave its recommendation an “I” for insufficient, rather than a grade (A, B, C, D), which denotes the strength of the evidence in favor of or against a specific service—a nuanced difference. Moreover, despite limited data, there was little or no evidence that skin cancer screening causes significant long-term cosmetic or psychosocial harm.
It’s also important to note that the panel’s recommendations are for preventive services and, as such, do not apply to people experiencing signs or symptoms of disease. In this case, then, the Task Force’s recommendation does not apply to people with a history of malignant or premalignant skin lesions, for example, or to anyone already being monitored because they are at increased risk for skin cancer.
Skin cancer is the most common cancer in the U.S., with close to 10,000 people diagnosed a day. Of the main types, basal and squamous cell carcinomas are highly treatable and rarely fatal when caught early—but melanomas, which are the least common, are the most deadly. According to the Task Force, about 98,000 new cases of melanoma will be diagnosed in 2023, and an estimated 8,000 people will die from it. You can develop skin cancer no matter your skin tone, with your risk increasing with age, if you’re male (presumably because men have more sun exposure), and if you have a history of frequent sunburns.
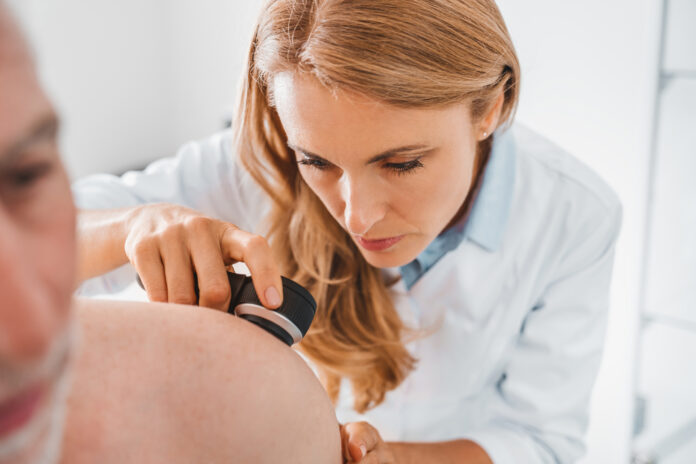
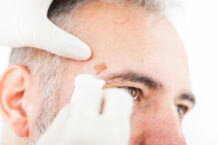
In a full-body skin cancer exam, the doctor does (or should do!) a visual scan of the patient’s body, from head to toe, with either the naked eye or a magnifying dermascope, typically going by the “ABCDE” rule, where they look for moles and other lesions with asymmetry, border irregularity, color that is non-uniform, diameter greater than 6 millimeters, and evolution over time (that is, the spot has changed appearance). The doctor may also look for an “ugly duckling” mole (one that is obviously different from others in the individual).
Whether you should continue to have routine skin exams is a decision best left to you and your doctor. But if you are at increased risk for skin cancer because you have a personal history of abnormal skin lesions or skin cancer or a family history of melanoma, or because you had a lot of sun exposure as a child or adolescent and experienced blistering sunburns, for example, then you should see a dermatologist for regular screening.
And whether your doctor does a regular skin exam or not, you should always take notice yourself of any new suspicious-looking skin lesions or changes to an existing lesion and report them to your doctor. When checking your skin, you can use the ABCDE and ugly duckling rules yourself, paying attention also to areas that aren’t typically exposed to sunlight, including the soles of your feet, the palms of your hands, and under your fingernails and toenails. For hard-to-see places, like your back, you can try to take photos (though admittedly that can be tricky, and the quality may not be very good) or have someone else check for you. In particular, photos can be good for tracking a single mole over time, to show your doctor.
Prevention is best. We can’t emphasize enough the importance of protecting your skin when outdoors, even on cloudy days. That means seeking shade whenever possible, using a broad-spectrum sunscreen with an SPF of at least 30, applying enough to adequately cover all sun-exposed areas (don’t skimp!) and reapplying it regularly as directed (including after swimming and heavy sweating), and wearing protective clothing, including a wide-brimmed hat. UV clothing that blocks the sun’s rays is a good investment. And we highly caution against indoor tanning beds, which, even if they don’t cause sunburns, increase skin cancer risk. For more tips, see our article Summertime Swim Tips: Cover Up!