You may think all you need to know about your bone health is your bone mineral density (BMD) score. And if it’s good, all is well. Not necessarily.
BMD, as measured by a DEXA scan (a type of X-ray), is only part of the picture. A bone that’s dense isn’t necessarily a stronger bone. Consider when fluoride was a treatment for osteoporosis. Though it was found to increase BMD, it also made bones more brittle and easier to fracture, presumably because it had a negative impact on what’s referred to as bone quality. After all, bone strength and its ability to resist fracture depends on not just the density of the bone but also its quality. And BMD is a measure of just the amount or quantity of bone, not the quality.
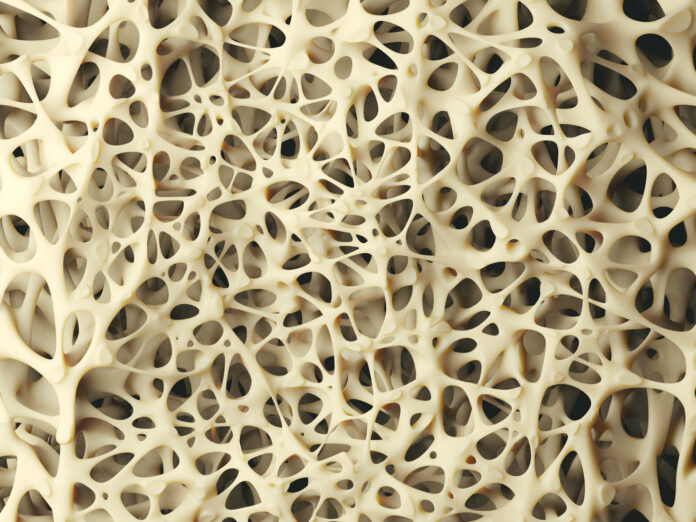
Bone quality refers to many other aspects of bone beyond its density, such as its microarchitecture, which means the patterns and formations in the tissues making up the bone, as well as the shapes of the bony material, the size and arrangement of the mineral crystals, and the quality of the collagen (a type of connective tissue). Good bone quality means that the bone has good tensile strength and is able to bend and flex to resist fracture.
In a study in Orthopedics and Rheumatology in 2018, researchers analyzed bone segments from people who had a hip replacement. They found that bone quality was a better predictor of the strength of bone than BMD.
Where BMD falls short
Even if BMD is helpful in predicting the risk of a fracture to some degree, there are many situations related to medical conditions, illnesses, or medications where this measure falls short. For example, for people with obesity, late-stage chronic kidney disease, or chronic inflammatory disease, and those who are taking steroids long term, their fracture risk is higher than what would be expected based on BMD alone.
Another example: Though people of Asian descent have BMD measurements similar to those of white individuals, they have about half the risk of hip fractures.
Age also plays a role in fracture risk despite the same BMD, as explained in a commentary in Kidney International in 2016. Take two white women with the same BMD but of different ages—one who is 60 years old and the other, 80. The younger woman has a lower incidence of hip fractures compared with the older woman. Specifically, a 60-year-old woman with a BMD T-score of –2.5 has an estimated incidence of hip fractures of 2.4 percent per decade, while the same T-score in an 80-year-old woman is linked with a fracture incidence of 6.1 percent per decade.
A better predictor of fractures?
If BMD isn’t always the most complete predictor of bone strength and fracture risk, is there something better? Some medical centers, such as Penn Medicine in Pennsylvania, offer an additional tool to estimate your bone quality. It’s referred to as the Trabecular Bone Score (TBS). This is not a separate scan and as such doesn’t add any more time or radiation to the test. Rather, it is specific (FDA-approved) software that generates additional data from the DEXA scan of your spine to provide an index of your bone’s microarchitecture.
A high TBS score reflects a strong bone with good bone architecture, while a low score indicates a bone that’s fragile. As you age, TBS scores tend to decrease, especially in women. A normal TBS score is above 1.350, while a score between 1.200 and 1.350 reflects some degradation of the bone’s microstructure. Anything less than 1.200 means the microstructure is degraded.
According to a 2020 review article that summarized the findings from six studies, a low TBS score among postmenopausal women was associated with 1.5 times greater fracture risk compared with women who had a normal score. The authors note that TBS can help determine the risk of having a bone fracture, but specify that it should be used along with BMD.
TBS plus FRAX: More alphabet soup
Though TBS can help predict fracture risk independent of BMD, it is usually used to adjust the FRAX score, says Risa Kagan, MD, an osteoporosis expert and a member of our editorial board. FRAX (Fracture Risk Assessment Tool) is used to predict an individual’s 10-year risk of suffering a major osteoporotic fracture, based on BMD scores plus clinical risk factors, including age, gender, parental history of hip fracture, alcohol intake, body mass index, and smoking history.
Adding TBS to the FRAX equation enhances the algorithm’s ability to predict fracture risk, studies have indicated. And it may be especially useful to do this for people who have osteopenia (low bone mass) to help in treatment decisions, according to clinical practice guidelines released in 2020—as opposed to in patients who have osteoporosis, for whom treatment is already indicated. TBS-adjusted FRAX may also be important in people with diabetes and primary hyperparathyroidism, “where FRAX without TBS may underestimate fracture risk,” the statement reads.
BOTTOM LINE: Measurement of bone quality with TBS is still something being done mostly in research, not clinical, settings—and traditional DEXA testing of bone mineral density remains the most practical tool we currently have for preventing future fractures, along with consideration of clinical risk factors. Still, you can talk with your doctor about whether you should get a TBS scan, if it’s available to you, as an add-on to your BMD testing to better gauge your fracture risk. Medicare recently started paying for TBS (in addition to its usual coverage of BMD testing). For how to possibly improve bone quality, see box.
Important for all DEXA testing—whether a TBS scan is added or not—is to use the same machine for repeat testing, or at least use a machine from the same manufacturer (Lunar or Hologic, for example); results can vary otherwise. That is, once you start testing, you should make every attempt to go to the same facility and make sure the machine is the same one or type as your last test. If the same machine is no longer available, or you must switch for other reasons, your next test will be considered a new “baseline.”
Most studies on bone health look at bone mineral density (BMD) and how that can be improved. There is far less research on what can preserve or improve bone microarchitecture, as an aspect of bone quality. But a few studies over the past decade or so suggest that some of the same measures that improve bone density may also improve bone quality.
-
High-impact exercise (such as hopping or jumping). A study in the Journal of Clinical Endocrinology & Metabolism of more than 800 young men found that activities that involve a lot of jumping (such as basketball or handball) or are explosive and involve quick turning and sprinting action (such as badminton or soccer) exert a high level of strain on bones, and this was linked with better bone quality compared with other weight-bearing or non-weight-bearing activities with lower levels of strain (including even jogging or weight training). A very small study of postmenopausal women, in Osteoporosis International, concluded that a six-month hopping program may also benefit some aspects of bone quality.
Though walking is a weight-bearing activity, it doesn’t appear to be high-impact enough to exert bone microarchitecture benefits, according to some preliminary research. But other activities that can fit the bill for involving sprinting or explosive movements are tennis, jumping rope, running stairs, and plyometrics workouts (which may include box jumps, squat thrusts, lunge jumps, and burpees).Because such high-impact, explosive movements and exercises can be risky if you have bone, mobility, or balance issues, it’s best to work with a trainer or physical therapist before attempting them on your own. Some require a fair amount of skill, coordination, and finesse.
- Medication. A review paper in the International Journal of Clinical Rheumatology noted that bisphosphonates (used to prevent or treat osteoporosis) and the estrogen modulator drug raloxifene (Evista, used for osteoporosis as well as for breast cancer prevention) preserve bone microarchitecture, while the osteoporosis drug teriparatide (Forteo), a synthetic form of parathyroid hormone, appears to improve bone microarchitecture.