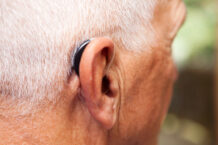
Starting after age 50, a significant proportion of people begin to experience progressive, age-related hearing loss. In the past decade or so, a major body of research has found hearing loss to be a risk factor for cognitive decline and dementia. This growing awareness helped spark efforts to make hearing devices more widely available and less expensive. Last August, the Food and Drug Administration issued final regulations governing the sale of over-the-counter (OTC) hearing aids, which can now be bought directly from retail outlets without a hearing exam, a prescription, or any audiology services.
The Wellness Letter spoke with audiologist Susanna Storm, Au.D., president and CEO of Blue Sky Hearing & Audiology in Berkeley, California. Dr. Storm originally planned to follow in the family business—her father was a dentist and her mother a dental hygienist, and they ran a practice together. But then she took an audiology course and simultaneously volunteered at St. Louis’s Central Institute for the Deaf—and immediately shifted gears. She received her doctorate in audiology in 2007 from Washington University in St. Louis.
The Wellness Letter: Can you explain why hearing loss might lead to cognitive decline?
Dr. Susanna Storm: We know through the extensive amount of research available that untreated hearing loss has connections with cognitive decline. As we age, it is common for hearing loss to occur. This age-related hearing loss is known as presbycusis. About a decade ago, Frank Lin, a physician and researcher at Johns Hopkins, analyzed the MRI results from the Baltimore Longitudinal Study of Aging and found that study participants with hearing loss at the start of the study had accelerated rates of brain atrophy compared to those with normal hearing. He concluded that shrinkage in the auditory cortex, which is the area responsible for speech and sound, may be due to lack of stimulation.
Research has also found that high-frequency hearing loss can lead to degradation of gray matter within the auditory cortex—the part of the brain that processes sound. As the auditory cortex has less stimulation over time, gray matter can reduce over time. That’s why I’m really encouraging patients to have their hearing tested sooner rather than later. The other reason is that although the research shows that untreated hearing loss can result in a decline in auditory processing, it also shows that hearing aids can improve brain function.
WL: What are the implications of this in terms of screening and treatment for hearing loss?
SS: Since we know that cognitive function can be impacted by untreated hearing loss, it makes sense that we should have our hearing tested before something is wrong. Think about what we do with vision. We start testing children’s vision when they are young because if there are any vision difficulties, it’s important to treat them immediately. This prevents vision from affecting additional areas of their life. Under Universal Newborn Hearing Screenings, implemented in 1992, all newborns in the U.S. must have their hearing screened prior to leaving the hospital. In California, school-age children have mandated hearing screenings in kindergarten, 2nd grade, 5th grade, 8th grade, and 10–11th grades. Many of my patients report that their last hearing test was performed in school.
As we can see from the research, early detection and intervention is key to maintaining long-term auditory function. When no known hearing problems are detected, I recommend having a hearing test performed every five years until 50 years of age and every three years following. Once hearing loss is detected, I recommend treatment options and annual hearing tests to monitor progression.
WL: How widespread is age-related hearing loss?
SS: Statistics show that 25 percent of people between the ages of 65 and 74 have hearing loss. And then when you look at individuals from 75 on, half are going to have disabling hearing loss. So in general, the earlier we can establish a baseline, the better. If I have a patient who is 50 and we establish a baseline and it’s completely normal, I’ll say, “Great, I’ll see you in three years.” Once hearing loss is detected, we will then begin testing on an annual basis.
Hearing tests are important not only to diagnose and treat hearing loss, but also to shine light on other potential issues. Certain types of hearing loss may be a red flag for other health-related issues. Low-frequency hearing loss can be associated with heart disease, high-frequency hearing loss can be associated with noise exposure, presbycusis, or ototoxicity [damage to the ear from medications or other substances]. Mid-frequency hearing loss may be due to possible genetic predisposition to hearing loss. When the ears do not decline at the same rate or severity, this can be due to possible retrocochlear pathology [hearing loss related to problems with the auditory nerve or the brain] or a benign tumor. Hearing tests are an important tool for prevention as well as a unique view into other parts of the body.
WL: If someone has a mild hearing loss, what is the next step?
SS: We cannot always say that borderline or mild hearing loss is in fact “just mild.” This is all dependent on how the individual is hearing overall. I have seen some patients with borderline or mild hearing loss that have difficulty understanding speech in quiet or background noise, so yes, it makes sense to pursue hearing aids or assistive technology to improve speech understanding. Sometimes there may be a very mild loss, but they’re not reporting any difficulties with comprehension. Once diagnosed, those who have borderline or mild loss but do not report any difficulties will be annually tested.
Knowledge is power. Once patients know what to look out for, like difficulty hearing when it’s noisy or difficulty understanding speech clearly, they will continue to monitor their hearing ability in their own listening environments while we monitor their hearing annually. When we get to the point where individuals are starting to notice some difficulties with their hearing and do become a candidate for a hearing device, we’re addressing it earlier rather than later. Just like we discussed at the beginning, we want to make sure we address hearing loss ASAP because we want to prevent decline in the auditory cortex.
WL: Before we talk about the various devices, what do you advise people in general about noise exposure?
SS: Hearing protection is the best thing that individuals can do to prevent hearing loss. There are things that can affect our hearing but are out of our control—our genetic predisposition, certain medications we take, or if we are lucky enough to have had many birthdays. The one aspect we can control in regard to our hearing is protecting our ears from loud sounds. I always recommend hearing protection. In fact, I give it out like candy at my office, because it’s just so important.
And there is something that I am finding clinically that is new and exciting. More and more younger adults are scheduling appointments with our office for custom hearing protection and hearing tests. That is great news as it shows that younger people are thinking about their hearing earlier and wanting to make sure they protect it in any way they can.
WL: Hearing protection means earplugs?
SS: It could be over-the-counter earplugs made of foam, but it could also be custom musician earplugs, sleep plugs, or swim plugs. Custom musician plugs are great for individuals who attend concerts or play music themselves. Non-custom earplugs change the frequency makeup of music and can distort the balance of sound. Musician earplugs have a filter in them to take down all the frequencies equally. So you still maintain the same balance and quality of music, but at a level that is safe for your ears.
WL: And is the issue with noise about one-time exposures or prolonged exposures?
SS: It all depends on the intensity of the sound. The lower the intensity, the longer we can be exposed to it without resultant hearing loss. The higher the intensity, the less time we can be exposed before it causes hearing loss. OSHA [the Occupational Safety and Health Administration, which regulates workplaces] requires employers to provide hearing protection when the employee is going to be exposed at or above 85 decibels [dB] for eight hours or more. Remember the idea of intensity. You may be able to be exposed to 80dB of noise for eight hours safely, but it only takes one gunshot, which is typically 140–165dB, to cause hearing loss if the shot was close to your ear.
WL: And what about while flying or riding the subway? How noisy is that?
SS: On a flight, the engine noise is not generally at a level that’s damaging to your hearing when you’re inside the plane. With that being said, I wear ear plugs on all flights because for me engine noise is constant and exhausting to hear over a long period of time. I find there are times when I wear hearing protection as it calms the world and improves my mental focus. I definitely recommend hearing protection when riding rapid transit because sometimes it can be very loud and, at times for me, painful. If I am on public transportation, you’ll always see me with hearing protection.
WL: So let’s move on to the devices. First, let’s distinguish between hearing aids and amplifiers, which is a less expensive category.
SS: Yes, there are two different categories. There’s what are called personal sound amplification products, or PSAPs, which increase the volume of all sounds in your environment. There’s no distinction between what’s important and what’s not—personal sound amplifiers just turn things up like your television volume. Unlike hearing aids, they’re not designed to address an individual’s specific hearing deficits. On the other hand, these hearing devices have features such as noise reduction and speech enhancement to improve overall hearing and can be digitally adjusted for specific situations and needs.
WL: And then we have hearing aids, which are now being sold over the counter. What are those like?
SS: The introduction of over-the-counter (OTC) hearing devices means that hearing technology is available at a lower price point. Most insurance companies, including Medicare, do not provide benefits for hearing devices. By expanding the marketplace, more individuals with hearing loss will be able to get hearing aids. But there are some caveats: OTC devices are for those with mild to moderate hearing loss. According to FDA regulations, they are not for individuals who have more extensive hearing loss, and they are not intended for children under the age of 18. OTC devices are purchased and programmed by the consumer.
These devices would be best suited for those individuals with quiet lifestyles mostly involving being at home, watching television, having one-to-one conversations, or gathering in small groups, as only minimal adjustments can be made by the consumer. OTC devices are also more appropriate for individuals who can work with technology, since all programming, adjustments, and troubleshooting are performed by the consumer. If there is a problem, the consumer will need to troubleshoot and fix the problem or return the device to where it was purchased.
On the other hand, if an individual has difficulty hearing in more diverse environments, such as larger groups, with more background noise, listening to music, being in lecture halls, etc., or has more extensive hearing loss or wants to achieve their best hearing possible, hearing devices fit by an audiologist would be most appropriate. Hearing devices ordered from manufacturers and fit by audiologists are very different than OTC devices.
WL: Different in what way?
SS: First and foremost, audiologists will comprehensively assess hearing, discuss hearing needs and goals, assist in finding technology that is best suited for an individual’s lifestyle, program and verify the function of the devices, train the individual on care and use, counsel on Bluetooth technology, and perform routine care and maintenance to make sure the devices are maximized to their greatest potential. Secondly, this technology has many features to combat challenging listening environments, and the devices react to the surrounding world automatically without the individual having to make manual adjustments. There are features that maximize speech understanding and reduce background noise, and connect wirelessly with other technology in our world, such as cell phones, computers, televisions, remote microphones, etc. This type of technology opens up a world of options and solutions for individuals with hearing loss.