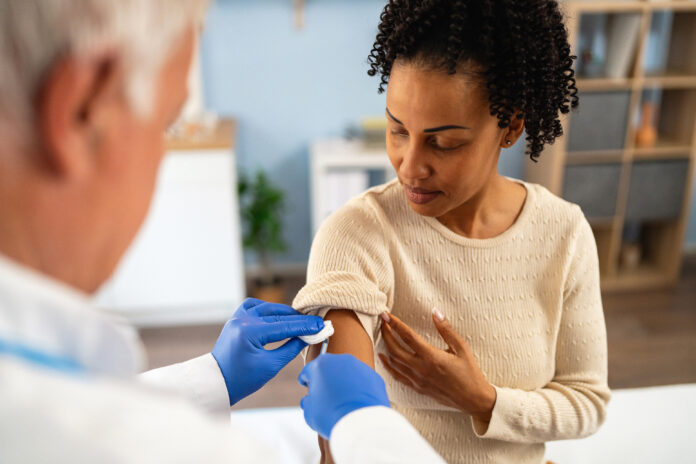
If you’ve been putting off getting a shingles vaccine, recent study findings might give you some extra incentive: That two-dose jab might not only ward off a painful case of shingles—it could also potentially delay or help prevent dementia.
Researchers found that older adults in Wales who received their routine shingles vaccination were 20 percent less likely to develop dementia over the next seven years, versus their unvaccinated peers. The protection could not be explained by other factors, such as differences in the two groups’ use of preventive medical care in general.
The study, published in April in the journal Nature, does not prove that shingles vaccination helps shield the aging brain. But it does build on previous research linking the vaccine to lower dementia risk, strengthening the case that the effect might just be real.
The shingles-dementia connection
First, here’s some background on why researchers are studying this question at all. Shingles is a painful rash caused by the chickenpox virus, varicella zoster. Once someone has had chickenpox, the virus continues to dwell in the body’s nerve tissue in a dormant state—but it commonly reactivates many years later to cause shingles. This is why shingles vaccination is recommended for everyone ages 50 and older, as well as adults whose immune system is weakened due to a medical condition or treatment.
While Alzheimer’s disease and other forms of dementia are very complex, researchers have long theorized that infections play a role in some cases. Herpes viruses, a large group of viruses that includes varicella zoster, are among the suspects. Scientists are still trying to understand how infections might contribute to dementia, but there is evidence that some viruses and bacteria can take up residence in the body long term and wreak havoc in several ways: promoting the buildup of the abnormal brain proteins seen in Alzheimer’s, feeding inflammation in the brain, or causing problems in the blood vessels that disrupt blood flow to the brain.
If that’s true, it begs the question: Can preventing those infections, or the reawakening of dormant infections, help lower the risk of dementia? In fact, a number of studies over the years have found a link between shingles vaccination and lower dementia risk. However, they were hampered by design shortcomings: The studies looked back at health records from vaccinated and unvaccinated people to compare dementia rates between the two groups. That’s a major limitation because there are many differences between people who opt to get vaccinated and those who don’t, and these types of studies cannot fully account for those differences.
The latest findings
In contrast, the new study took an alternative approach known as a “natural experiment.” That’s a study design that takes advantage of events that happen in the real world—like a policy change on vaccinations—to see whether that event had an effect on a particular health outcome.
Here’s what happened in Wales, where the study was set: When the Zostavax vaccine (the original shingles vaccine) became available there in 2013, government officials set a cutoff date for eligibility: People born on or after September 2, 1933, could get the vaccination, while those born earlier were ineligible. That allowed the researchers to compare Welsh adults who were born just one week apart, with the only major difference between the two groups being shingles vaccination rates: virtually nil, versus 47 percent. (Conversely, both groups had nearly identical rates of flu and pneumococcal vaccination, and similar rates of statin use for cardiovascular disease prevention.)
In addition to the 20 percent lower dementia risk seen in the vaccinated group, the researchers reported some other intriguing findings: There was no evidence that shingles vaccination helped ward off any other chronic medical condition (hinting that there’s a specific relationship with dementia). And among people who had shingles diagnoses in their medical records, those who had multiple bouts were at greater risk of dementia than those who had shingles only once.
There has been one other natural experiment on this issue—a study published last year in Nature Medicine that looked at the relationship between vaccination with Shingrix and dementia risk. Shingrix was approved in the U.S. in 2017 and rapidly replaced Zostavax because it is more effective at preventing shingles, and it can be given to immunocompromised individuals (Zostavax, a live-attenuated vaccine, cannot be used in these individuals).
That set up the basis for this study: The researchers compared dementia incidence among U.S. adults who were vaccinated with Shingrix in the three years after the switch against those who had received Zostavax in the three years before. On average, people who had received the more effective Shingrix vaccine lived longer dementia-free (roughly an extra six months), with age and other factors taken into account.
The Takeaway
While those two studies offer the strongest evidence yet that shingles vaccination might sway the likelihood of developing dementia, they still fall short of definitive proof. The researchers on the Wales study have said they are aiming to conduct a clinical trial that will directly test the effect of shingles vaccination on dementia risk.
For now, you can focus on what is known. The Shingrix vaccine is over 90 percent effective at preventing shingles and postherpetic neuralgia, a complication that causes debilitating nerve pain that can persist for months to years. Based on studies so far, that protection lasts at least seven years in adults ages 70 or older with healthy immune systems. In other words, there’s already good reason to get the recommended two doses of Shingrix. Now we have growing evidence that there might be a bonus benefit for cognitive health, too.